All About Demodex Mites | What Are They & How Do You Get Rid Of Demodex Brevis?

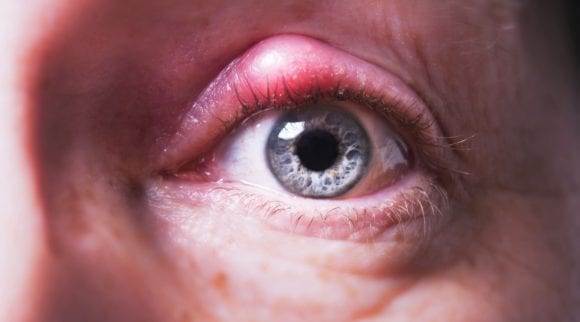
If you wake up to itchy eyes, a burning sensation, and a feeling that there’s something trapped under your eyelids that you can’t quite see or remove, you might have a Demodex Mites infestation.
What are Demodex Mites? They’re an eight-legged (yes, they are arachnids and are related to spiders) ectoparasite (living on the surface of the host) that can reside in our hair follicles and sebaceous glands. There are 65 varieties of Demodex Mites, but fortunately only two, Demodex brevis (D. brevis) and Demodex folliculorum (D. folliculorum), actually live on humans. Both microscopic mites live in human hair follicles, including eyelashes, eyebrows, nose and ear hair, scalp, chest hair, underarms, etc.
Even if you don’t have any symptoms, you can still have these mites. In fact, on about every tenth eyelash, one or more Demodex Mites can be detected even in healthy, asymptomatic patients. Demodex Mites occur almost equally in males and females, although more men than women suffer from symptoms and their occurrence seems to be age-related. A study by Junemann showed that Demodex Mites are found in 25% of 20-year-olds, 30% of 50-year-olds and 100% of patients older than 90 years.

Read More on Demodex Mites Here
Fortunately, the “gross” factor for these mites is small. The idea of mites living on your eyes is worse than the actual mite itself since they can only be seen through a microscope. However, many doctors will show their patients photos of the mites taken through a microscope so they can see it’s a very real creature and a health threat that needs to be addressed immediately, and aggressively.
If you do have a Demodex infestation, it’s important to treat it immediately. Not treating it can lead to:
- Clogged glands, preventing natural lubrication of your eyes
- Swelling and inflammation of the eyelid and eyes
- Thickened eyelids
- The appearance of scaly skin
Demodex Folliculorum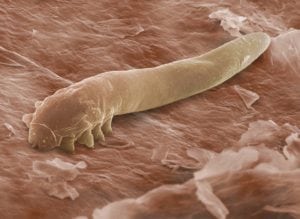
The D. folliculorum mite was first reported around 1840. This hair follicle mite is the only metazoan organism commonly found in the eyelashes and eyelids of humans. D. folliculorum is mostly found on the face and around the eyelids and eyelashes. It feeds on skin cells, whereas D. brevis feeds on oil called sebum in the oil gland cells.
D. folliculorum is different from other types of mites because it can actually increase the number of skin cells in hair follicles. This can give people the appearance of scaly skin. D. folliculorum is currently being investigated as a potential cause of rosacea. There is evidence that these mites can cause flare-ups if you have rosacea. The National Rosacea Foundation estimates that rosacea patients have up to 18 times more D. folliculorum mites than patients without rosacea.
According to an article in New Scientist, these mites crawl around your face at night to mate, then crawl back into your pores to lay eggs and die. Unfortunately, these creatures don’t have an anus, which means they don’t poop. Their abdomens just continue to swell until they die in your pores. As they decompose they release a lifetime of poop onto your skin, pores or eyelashes. All the more reason for immediate and aggressive treatment! Yikes!
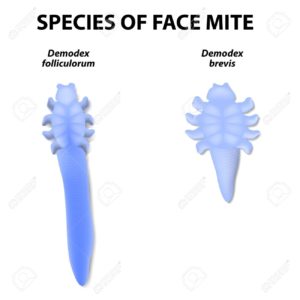
Demodex Brevis
Demodex brevis is about 0.2mm long, and is found in lash follicles, meibomian glands and Zeiss glands. It tends to inhabit sebaceous glands either singly or in small numbers rather than in a colony or group of mites. D. brevis appears to thrive on skin lipids, but its presence is often associated with dry skin.
This particular type of mite has been shown to cause plugging of the meibomian glands. Meibomian (“my-BOH-mee-an”) refers to a particular type of gland in the eyelids. There are about 25 to 40 meibomian glands in the upper eyelid and 20 to 30 in the lower eyelid. These glands secrete oils onto the surface of the eye that help keep our tears from evaporating too quickly.
Symptoms of Demodex Mites in Humans
Should you be worried about Demodex Mites if you have no symptoms? Not really. It’s actually common to have small amounts of these microbes on your body. Most people never realize they have Demodex Mites living in their follicles because they don’t have symptoms. Many people only learn they have them when they are being tested for other skin conditions or issues, such as dry eye disease. Your doctor will make a Demodex Mite diagnosis by analyzing a skin sample under a microscope, to confirm the presence of the mites, but it’s not necessary for a person to get tested unless they experience symptoms or complications.
Patients with mite infestation may complain of itchiness that is worse in dim light, especially after going to bed or upon awakening. Having  brittle eyelashes, or eyelashes that break easily or are easily pulled out of, or fall out of the eyelid, are also tell-tale signs of a mite infestation. Dry eye symptoms and plugged or clogged meibomian glands are also a sign there may be a mite infestation. There are many factors that contribute to infestation, but the main one seems to be that mite infestation tends to increase with age. Lid biopsies show that 84 percent of individuals over 61 have the condition.
brittle eyelashes, or eyelashes that break easily or are easily pulled out of, or fall out of the eyelid, are also tell-tale signs of a mite infestation. Dry eye symptoms and plugged or clogged meibomian glands are also a sign there may be a mite infestation. There are many factors that contribute to infestation, but the main one seems to be that mite infestation tends to increase with age. Lid biopsies show that 84 percent of individuals over 61 have the condition.
Other symptoms of a Demodex Mite infestation include: reddened, crusty, itchy, burning eyelids. Some people may find the skin on their eyelids thickening as well.

How are Demodex Mites Diagnosed?
Dermatologists are the doctors most likely to diagnose Demodex Mites, although many eye doctors can also diagnose the condition. Once diagnosed they can refer you to a specialist (dermatologist), or treat it themselves.

Demodex brevis is usually diagnosed with a biopsy. A biopsy involves taking a small skin sample and checking it under a microscope. Your doctor will also ask about symptoms and look for other signs of the mites, such as scaly skin. Demodicosis will be diagnosed if there is a high level of mites in the follicles
While many people have these mites but don’t have symptoms, large infestations of the mites may lead to symptoms such as:
- Red skin
- A rough texture to the skin, like sandpaper
- A burning sensation in the skin
- Symptoms can be experienced in any area because D. brevis will inhabit any of the body’s oil glands, but the head and chest are where most symptoms begin
- Itchy rash
- Demodex brevis has also been known to make skin conditions such as eczema and rosacea worse.
Left untreated, Demodex Mites can lead to Demodicosis, an inflammatory disease, with symptoms including:
- Color changes in the skin (Rosacea)
- Scaly skin
- Red skin
- Sensitive or irritated skin
- Itching
- Rash
- Eye irritation
- Thickening of the eyelid
- Loss of eyelashes
Inflammation of the eyelids is called Blepharitis (blef-uh-RYE-tis). Blepharitis usually involves the part of the eyelid where the eyelashes grow and affects both eyelids. Blepharitis commonly occurs when tiny oil glands located near the base of the eyelashes become clogged. Although, other health conditions can also cause clogging. Your doctor can best determine what the cause of your eye inflammation is.

Are Demodex Mites Contagious?
Like lice and other body mites, Demodex Mites can spread from person to person, although they are not “contagious.” They are, however, easily spread within families and among people living together, or sharing makeup, towels, washcloths, and personal items. D. brevis can also be spread by contact with other people through sex, hugging, and physical intimacy. Once on the body, the mites feed off the oil gland cells that are attached to hair follicles. They can also be found on bedding, pillows, clothing, and shared personal items.
Risk Factors For Getting A Demodex Mite Infestation

Because these mites are very common, anyone can have D. brevis, but there are some factors that increase the likelihood and severity of you getting a Demodex infestation that causes symptoms and problems.
These risk factors include pre-existing conditions such as:
- Acne - People who suffer from acne produce three times the amount of sebum of non-acne sufferers, creating a sebaceous feast for Demodex Mites. However, it is not clear if the acne comes first, and then the Demodex Mites, or if the mites come first and then the acne follows. Either way, it’s the amount of sebum that the mites feast on that is the issue.
- Alopecia
- A weakened immune system, such as people with HIV
- Eczema
- Wearing contact lenses
- Hair loss
- Corticosteroids, such as prednisone
- Some people are genetically susceptible to D. folliculorum and thus more sensitive to the presence of the mites
- A history of cancer or liver disease
- Improper hygiene (not washing your face regularly)
- Immune deficiency
- Women who wear mascara or a lot of eye makeup tend to have a higher prevalence of Demodex mites on their eyelashes.
- Not washing your face at night or sleeping with makeup on
- Oily skin
- Rosacea
- Aging - older adults are also more likely to have Demodex mites and experience complications, such as demodicosis
- Young adults - Demodex brevis is most common in people aged 20 to 30 years because sebum levels are at their highest during that period. The mites are rarely seen in children under 5 years of age due to low sebum production.
- Being male - D. brevis and D. folliculorum are more common in men than in women, although it is not clear why this is the case.
Demodex Mites and Rosacea
Some research has found a link, or greater prevalence of Demodex Mites in people with Rosacea, a skin condition that causes flushing, redness, and bumps across the nose, cheeks, chin, and forehead. It usually strikes after age 30 and affects more women than men. It tends to flare in response to certain triggers, like sun exposure or emotional stress.
Not everyone believes there is a link between Rosacea and Demodex Mites, but research shows there is some connection. Kevin Kavanagh of the National University of Ireland, in Maynooth, believes Rosacea is caused by the Demodex who eat sebum, or facial oil, and colonize your face at puberty. The reason some doctors don’t believe that mites cause Rosacea is that the condition often improves with antibacterial drugs that don’t affect the mites, such as tetracyclines.

However, Kavanagh thinks this is because Rosacea is caused by a reaction to bacteria in the mite’s feces. Because the Demodex Mite does not have an anus and therefore cannot get rid of its feces, their abdomen just gets bigger and bigger. When they die and decompose they release their feces all at once in the pore. This, says Kavanagh, can be enough to trigger an immune reaction, inflammation and tissue damage if there is a large enough infestation.
Changes in the skin brought on by age, stress, or illness sometimes allows the population of Demodex mites to swell, Kavanagh says. Research shows that people with rosacea have more than 10 times as many Demodex mites on their skin as people without the condition.
“When each of those [mites] dies, they release bacteria into the skin,” he says. Those bacteria trigger an immune reaction that causes redness and inflammation of the skin. The mites themselves don’t seem to be harmful, Kavanagh says. It’s the bacteria they have inside their bodies.
Other researchers believe Demodex brevis may also play a role in ocular rosacea, a subtype of rosacea that involves irritation of the eyes. While researchers have long debated whether the increased prevalence of mites in the facial skin is a result of rosacea, more recent research has pointed to the possibility that the mite may play a role in its development because of the eyelash irritation and presence of the mites in those with this form of Rosacea.

The Life Cycle of the Demodex Mite
The life cycle of a typical Demodex mite is about two-to-three weeks, or 14-18 days. A female Demodex mite will lay 15 to 20 eggs inside the hair follicle near the sebaceous glands. The eggs develop into larvae, which eventually become an adult eight-legged mite. The adult male Demodex mite will leave the follicle in search of a mate, while the adult female mite remains in the follicle. The mites are capable of walking approximately half an inch an hour. It doesn’t sound like much, but over an evening they can infest your head quite easily. They also tend to be more active in the dark, so while you’re sleeping, they’re on the move.
Once it gets light, the Demodex Mite retreats back into the hair follicle, skin, or eyelashes where they wait for darkness again before coming back out to feed and move around.
How to Get Rid of Demodex Mites
There are a variety of ways to get rid of Demodex Mites - through traditional medical treatments, and some home remedies that are similar to medical treatment. All of these methods involve eliminating the existing Demodex Mites, preventing the spread of new ones, and treating the inflammation they have caused.
How to Prevent Demodex Mites
If you know someone who has these mites, or you’ve just discovered them by reading this article, you know you don’t want them yourself. So how can you keep from getting a Demodex Mite infestation? Don’t get old. The alternative to aging is, well, not aging, and being dead won’t matter. If you age you’re much more likely to get an infestation unless you follow these tips:
- Clean your eyelids regularly with a hypochlorous acid eyelid cleanser, like Heyedrate Lid & Lash Cleanser. Think of it like brushing your teeth, keeping your eyelids clean will help prevent symptoms of demodex and prevent overgrowth.
- Wash your face twice daily and body once daily with a tea tree oil soap.
- Exfoliate: By periodically exfoliating your skin, you clean out your pores and remove the dead skin cells that mites love to feed on.
- Don’t share towels, washcloths, hair brushes, combs or other personal care items with anyone - no matter how clean they say they are, or seem to be.
- Don’t share makeup with anyone.
- Throw away makeup or replace it every 30-to-60 days - especially mascara.
- Wash your makeup off every night.
- Replace your pillows-throw them away and get new ones every six months if they’re plain old polyester pillows, and every 18-24 months if they’re memory foam pillows. You can extend the use of your pillows and cut down on mites by using dust mite pillow covers. Yes, they really do work. You can use them on your mattress and pillows.
- Become a clean freak. Eliminate clutter as that only attracts mites of all kinds
- Mix up your own mite spray using Tea Tree Oil (also known as Melaleuca Oil). Thanks to its antibacterial, antiviral and antifungal properties, it will eliminate dust mites, along with other allergy-inducing bacteria, viruses and fungi. Eucalyptus oil is another fantastic option, with proven mite-killing properties. Blend two cups of distilled water with two teaspoons of essential oil and decant into a dark-colored spray bottle. Use this blend when wet-dusting, or as a mite-killing spray for fabrics, bedding and carpets. Remember to shake before each use to distribute the oil.
- Always wash your sheets, blankets, and bed clothes in hot water and dry them on the highest heat settings to kill any mites
- Lower the temperature and humidity in your home. Keeping your home comfortable and dry is key to mite control - including dust mites!

Medical Remedies:
Whether you depend on a doctor, or try to treat mites yourself, the goal is 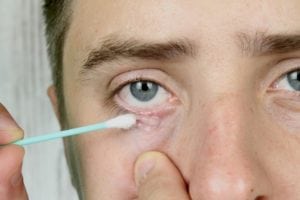 the same: treatment of mite infestation requires killing the adult mites and getting rid of the eggs before they hatch. In-office treatment by a doctor will involve carefully swabbing alcohol or diluted tea-tree oil on the eyelid margin three times per week. It’s important that these materials do not contact the cornea. This is followed up by in-home therapy by the patient. The in-home treatment usually includes cleaning your eyelids twice daily using a hypochlorous acid eyelid cleanser, like what was mentioned above, Heyedrate Lid and Lash Cleanser.
the same: treatment of mite infestation requires killing the adult mites and getting rid of the eggs before they hatch. In-office treatment by a doctor will involve carefully swabbing alcohol or diluted tea-tree oil on the eyelid margin three times per week. It’s important that these materials do not contact the cornea. This is followed up by in-home therapy by the patient. The in-home treatment usually includes cleaning your eyelids twice daily using a hypochlorous acid eyelid cleanser, like what was mentioned above, Heyedrate Lid and Lash Cleanser.
Both the doctor and patient will then coat the eyelid margins with a viscous ointment. These ointments appear to inhibit the reproductive activity of the adult mites and cut off oxygen to other mites trapped in hair follicles.
A 4% pilocarpine gel also works well, and this must be gotten from your eye doctor or dermatologist. Like other ointments, it works by interfering with the mite’s respiration, suffocating them. However, pilocarpine can cause severe problems, including retinal tears and detachment in some individuals. Patients should apply it directly to their eyelid with a cotton-tipped applicator.
Home Remedies:

Gently scrub your skin, eyelids, and eyelashes with a tea tree oil soap. Tea tree oil is known to kill Demodex. Then, use a hypochlorous acid eyelid cleanser to remove any of the bacteria that the mites would feed on. It is not recommended to apply diluted tea tree oil to kill any eggs left behind, because this could potentially burn the eyes if you are unsure of the dilution ratio. Due its antibacterial and antifungal properties, tea tree oil is useful for topical (on the skin) treatments and cleaning. However, it is toxic when ingested as well. It cannot be applied directly to the skin straight out of the bottle either. It must be properly diluted to be effective and not dangerous.
Many home remedies also encourage use of over-the-counter products and various oils, solutions, and substances. Many of these have been shown to effectively, and quite quickly, kill Demodex Mites in test tubes, but AREN’T safe to use around the eyes:
- 100% alcohol 4 minutes
- 100% tea tree oil 4 minutes
- 50% tea tree oil 15 minutes
- 100% caraway oil 4 minutes
- 100% dill weed oil 14 minutes
While very effective, Caraway oil and dill weed oil are toxic to the eye and should not be used in, or around the eyes. Alcohol and undiluted Tea Tree Oil are also effective, but shouldn’t be used around the eyes. These things can be used on hair brushes, and to clean areas where Demodex Mites might be present. Rather than depend on these substances, it’s often safer, cheaper, and more effective to turn to over-the-counter remedies like:
- Heyedrate Lid and Lash Cleanser
- Heyedrate Tea Tree Oil Soap
- Demodex Face Cream
- OCuSOFT Lid Scrub Plus Cleaning Pads
- Fischer Premium, Purified, Non-Irritating & Hypoallergenic Eyelid Wipes
- Cliradex Natural Eyelid, Eyelash, and Facial Cleansing Towelettes
- We Love Eyes - All Natural Tea Tree Eyelid Foaming Cleanser/Wash
- 20% Desert Essence
Tea Tree Oil and Demodex Treatment
Tea tree oil (TTO), also called melaleuca oil, is an essential oil that comes from steaming the leaves of the Australian tea tree. It’s very effective for a variety of health conditions. There is so much interest in the properties of tea tree oil that a research group has been created within the School of Biomedical, Biomolecular and Chemical Sciences at The University of Western Australia.
When used topically (on the skin), tea tree oil is believed to be antibacterial. Tea tree oil is commonly used to treat acne, athlete’s foot, lice, nail fungus and insect bites. External application of undiluted tea tree oil and/or at inappropriate high doses has been associated with toxicity, including death, in cats and other animals.
Tea tree oil is available as a pure, essential oil. It’s also used in many over-the-counter skin products, including soaps and lotions. Tea tree oil should not be taken orally. If swallowed, it can cause serious symptoms.

Click here to purchase tea tree oil.
Tea tree oil can help get rid of acne-causing bacteria, one of the risk factors for Demodex. Add 1-3 drops of tea tree oil to your cleanser or moisturizer and mix thoroughly. A drop or two of tea tree oil can also be mixed with a teaspoon of coconut oil and applied to your face. Use a cotton swab to apply the mixture to your face and let your skin absorb it.
Before applying tea tree oil on larger areas of the body, it is important to test for allergic reactions to it. Place a small amount of diluted Tea tree oil on a patch of skin. If you are allergic you will have a reaction - such as redness, swelling or itching at the site. If this happens, discontinue using the oil and consult a physician for an alternative product.
- There is good scientific evidence that tea tree oil is effective for treating acne, however, prepubescent boys should avoid using tea tree oil as it could lead to the growth of breast tissue.
- If you are pregnant, breastfeeding, or undergoing childbirth you need to avoid topical use of tea tree oil. It may decrease the strength of your contractions.
- If you have a known allergy or sensitivity to tea tree oil, Balsam of Peru, benzoin, colophony (rosin), tinctures, eucalyptol, or plants of the myrtle family, you should not use tea tree oil.
- Women should not apply tea tree oil to the breast area because it may have hormonal properties.
- If you have linear IgA, an immune disease, you should not use tea tree oil as it can cause blisters.
Tea Tree Oil can also be deadly to cats, dogs, and animals as they end up ingesting any topical application when they lick it off of their bodies while grooming.
Demodex Treatment
Demodex treatment is fairly straightforward. Your doctor’s goals will include:
- Eradicating the adult mites and their offspring
- Prevention of further mating and the spread of more mites
- Avoiding re-infestation from other sources (bedding, etc.)
- Alleviating the patient’s symptoms
Treatment lasts for six months, or indefinitely if there is an ongoing problem. It involves committed care at home to ensure that the mites are eliminated and don’t spread. That’s why it’s important the patient understands, and sees, what’s really happening to their eyelashes.
Initial Treatment
After diagnosing your Demodex Mites, your doctor will most likely begin your initial treatment in his/her office. This will involve an in-office lid scrub/débridement. It sounds scarier than it is. This process involves the doctor using a cotton tip applicator dipped in a long-lasting anesthetic to numb the eyelid area. Then they will attempt to thoroughly débride (rub away or remove) the mites from the lashes and eyebrows with a cotton tip applicator soaked in a solution of 20% to 50% tea tree oil.
Tea tree oil has excellent concentration-dependent Demodex-killing properties. While 100% tea tree oil solution is very irritating, once diluted in coconut, macadamia or walnut oil, it’s very soothing and still very effective.
A commercially available tea tree oil, 20% Desert Essence (www.desertessence.com) is also effective. This solution irritates the mites and stimulates them to come out of the follicle. This process is repeated after 10 minutes.
Next, an antibiotic/steroid ointment is applied to help keep the mites from moving to other areas of the head and face. It’s thought the ointment also suffocates them. The steroid calms the inflammation and irritation created by the tea-tree oil solution and debridement. It also helps suppress a possible inflammatory cascade associated with the decaying mites.
Patients can expect to return every two weeks to repeat the treatment until the mites are gone.

Removing Demodex Mites at Home
Treatment for Demodex Mites doesn’t end at the doctor’s office. Once patient’s return home the “great purge” of potential reinfestation begins.
- Immediately wash all your sheets and pillow cases in hot water

- Dry all bedding on the hottest “high” dryer setting
- Discard all bed pillows
- Do not use makeup for at least one week
- Discard all old makeup
- Use tea tree soap on their face and consider using tea tree hair shampoo as well
- Make an appointment for the patient’s spouse and children to have an evaluation, as they are frequently also infested.
Myths and Facts About Demodex Mites and Treatment
There are a lot of rumors, myths, and misconceptions about Blepharitis (inflammation of the eyes) and Demodex Mites you may hear from friends and family. Here are some of the more popular myths, and the actual facts:
MYTH: Eye inflammation due to mites is rare.
FACT: Recent studies and meta-analysis of patients show that inflammation of the eye in 44% of Blepharitis patients is due to Demodex Mites with the prevalence of mite infestations increasing dramatically as people get older. In fact, 100% of patients aged 70 years and older are estimated to carry a colony of 1000 to 2000 mites.
MYTH: Old people don’t get Demodex Mites.
FACT: Actually, they do! The rate of Demodex Mite infestation increases with age, being observed in 84% of the population at age 60 and in 100% of those older than 70 years. Many of the eye problems and inflammation issues the elderly report may be Demodex Mites, not simply old age or other issues. If you or someone you love is over the age of 50, definitely ask your doctor to check for Demodex Mite infestation.
MYTH: Demodex Mites Cause Baldness
FACT: While Demodex Mites do feed on, and destroy the root of hair follicles, it’s not yet believed or proven that they cause baldness - like Alopecia. Baldness is typically a genetic or disease-driven condition, and researchers believe that while Demodex may play a role, or be attracted to or found in certain kinds of baldness, they’re more opportunistic than causative factors.

MYTH: Demodex Mites cause Rosacea
FACT: The connection between rosacea and Demodex mites is controversial and still being studied, however, skin mites have been connected to creating inflammatory skin diseases like Rosacea. Researchers believe that rosacea is not caused by the mites themselves, but from the bacteria in the feces that they carry.
A 2010 research analysis found that rosacea sufferers are almost eight times as likely to have a Demodex Mite infestation than someone with normal skin. The researchers concluded that an association exists (not necessarily causation). The study also found that the degree of infestation played a bigger role in rosacea development than did simply having an infestation.The take-away to this evidence is that reducing Demodex levels in a person with Rosacea can only have a beneficial effect on the condition.
MYTH: There aren’t many effective treatments for killing Demodex mites.
FACT: While Demodex Mites may be resistant to a wide range of antiseptic solutions and other traditional treatments, such as eye drops and wipes, there are many effective treatments that help both the symptoms and the problem of mites. Tea tree oil is a known killer of demodex, and many products exist out there that can help.
MYTH: 4-Terpineol, the key constituent of Tea Tree Oil, and pure Tea Tree Oil are equally effective in eradicating Demodex.
FACT: A recent study showed that 4-Terpineol is the ingredient in Tea Tree Oil that has been shown to be effective in treating Demodex Mites. It’s more effective than Tea Tree Oil alone.
There are also ingredients in Tea Tree Oil that limit its overall effectiveness and are known to cause irritation.
MYTH: Using 100% Tea Tree Oil is safe and effective.
FACT: Pure strength Tea Tree Oil can be dangerous, as well as irritating near the eyes. Cliradex®, a contains 4-Terpineol, which is clinically proven to kill Demodex mites better than Tea Tree Oil alone, and at a concentration low enough that it doesn’t irritate the eyes. Cliradex® is available over the counter and is a natural eyelid cleanser.
There are also dozens of other over-the-counter products that are very effective in treating Demodex Mites, many with appropriate and safe levels of Tea Tree Oil and 4-Terpineol.
Researchers report that among a total of 15 major ingredients in Tea Tree Oil they identified Terpinen-4-ol as the most potent (i.e. most active) ingredient based on the dose-dependent survival time measured by an in vitro killing assay. Using products that have 4-Terpinen without the other irritating ingredients found in pure Tea Tree Oil can be even more effective, and less irritating to the user.

MYTH: Your doctor needs a microscope to diagnose Demodex.
FACT: Although it’s helpful to have a microscope to verify or confirm a Demodex infestation, it’s not necessary. Doctors are able to diagnose Demodex by looking for clinical signs such as “cylindrical dandruff” and the absence of eyelashes. Cylindrical dandruff is a clear tubular cuff of skin and bacteria that is attached to the base of the eyelid and encircles the eyelash base. Research shows that cylindrical dandruff is pathognomonic for Demodex.
MYTH: Other people can tell you have Demodex Mites and will avoid you.
FACT: Even you and your doctor need a microscope to see Demodex Mites. It’s not likely anyone else will know you have them unless you share that information with them. Your red, itchy eyes can be attributed to allergies or a variety of other causes. So, don’t worry. People won’t run away in fear just by looking at you. Besides that, almost 100 percent of people have these mites living on their bodies. The mites don’t become an issue until they reach large enough numbers for doctors to term them an “infestation.”
MYTH: It’s traumatic to learn you have mites on your lashes.
FACT: Learning that you have mites on your eyelashes or other parts of your body CAN be very scary if you don’t understand what a mite is, or how it causes irritation, or how to manage or cure it. Educating yourself is the first step to eliminating fear about your condition. While it may be traumatic for some, that can be relieved through education, treatment, and prevention.
MYTH: Demodex Mites will make you go blind if left untreated.
FACT: Some people’s vision may be compromised due to a Demodex Mite infestation, but this would be due to later effects of the Demodex, such as dry eye disease. These mites may affect the tear film of the eyes, causing your vision to blur. Fortunately, this is temporary, and once the infestation is cleared up, your vision will return to normal.
New Developments to Help Those Suffering with Demodex Mites
Michele Green, MD, a dermatologist at Lenox Hill Hospital in New York City, like Kevin Kavanagh, PhD, a biologist at the National University of Ireland, Maynooth in Kildare, Ireland believes the mite theory fits many features of the disease. She says many people with rosacea notice that their skin gets worse after exposure to heat and humidity, conditions that also help mites thrive. Green and Kavanagh aren’t alone. Pharmaceutical companies are taking note as well. Galderma, the company that makes Metrogel, a topical antibiotic often prescribed to treat rosacea, is reportedly testing a product that targets Demodex mites.
Other researchers have found that, “Terpinen-4-ol was the only ingredient that is ranked as #1 according to both relative abundance and relative potency, suggesting that it is primarily responsible for TTO’s Demodex killing effect. Not surprisingly, Terpinen-4-ol was the only ingredient that exhibited a killing effect at a concentration as low as 1% in mineral oil. Furthermore, the potency of Terpinen-4-ol at a given concentration was greater than TTO at an equivalent concentration.”
Biohacking Demodex Mites
Some sufferers have resorted to what they call “Biohacking” the Demodex Mite. This means eliminating sugar consumption, depression, stress, hair products, gluten, and other things. They also suggest controlling the mites by always using mite killing oils in your daily cleaning products:
- Tea tree oil (For oily skin/scalp)
- Castor oil (For dry scalp)
- Mint oil cools down the scalp and might help with dandruff
- High-frequency skin care machine (Ozone Therapy)
- When washing your clothes, add 10–20 drops of tea tree oil to the detergent in the washing machine.
- Have a few clean cotton fabrics to use on top of your pillowcase, to make sure your skin rests in a clean place during the night
- Add a few drops of tea tree oil to a cotton ball and clean your cosmetic brushes, sunglass frames, glasses frames, etc.
- Clean your bath towels and bed sheets more frequently
Good News for Demodex Infestations
The good news for those suffering from Demodex Mites is that the infestation can be cured. Follow your doctor’s treatment regime and eliminate sources of reinfestation - like pillows, bedding, clothes, etc. You could be free and rid of the problem within months, and experience relief within weeks.
The problem, doctors say, is that patients tend to stop treatment, cleaning, and maintenance of the infestation once they start experiencing relief from the symptoms. The most important thing anyone can do is to ensure they strictly follow the cleaning routine for six months, then make the preventive practices part of their daily routine.


 (4 votes, average: 4.50 out of 5)
(4 votes, average: 4.50 out of 5)